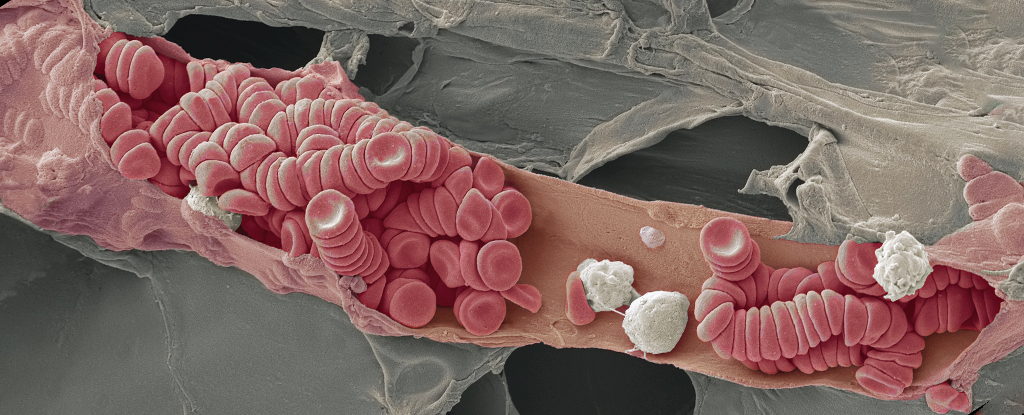
A common blood disorder associated with an increased risk of several diseases unexpectedly appears to lower the risk of Alzheimer’s disease.
People with clonal hematopoiesis of undetermined potential (CHIP) are 10 times more likely develop blood cancer and twice as likely to end up with heart and liver disease. So when Hind Bouzid, a cell biologist at Stanford University, and his colleagues set out to investigate how this condition got in the way of Alzheimer’s disease, it wasn’t the result they expected.
“We were surprised to find that CHIP was, in fact, associated with a significantly lower risk of Alzheimer’s disease,” say Stanford pathologist Siddhartha Jaiswal.
CHIP is often an age-related process. It arises when a blood cell parent (a stem cell) living in our bone marrow acquires a mutation that allows it to make mutated blood cells that are stronger than their peers. CHIP can form in otherwise healthy people and has no noticeable symptoms but exacerbates other conditions.
Because these blood cells can outnumber others, this genetically unique clone strain can replace nearly 100 percent of a person’s blood over time.
Analyzing the DNA of blood cells from 1,362 people with Alzheimer’s and 4,368 individuals without Alzheimer’s, Bouzid and the team found a 30-50 percent lower risk of Alzheimer’s in people with the blood mutation. This is a similar level of protection as a genetic variant known to reduce Alzheimer’s disease, Jaiswal explains.
It also suggests that the mutation affects tissues other than red blood cells. The researchers took a closer look, guided by previous research that previously found a link to other cells derived from bone marrow (collectively known as myeloid tissue).
Thanks to 12 donors, eight who had lived with CHIP and four without, the team identified such CHIP-carrying myeloid cells in brain tissue. Seven of the eight CHIP carriers had an increase in immune cells.
Usually it is the white blood cells that engulf foreign invaders in the brain microglia, which are produced in the brainconnective tissue. But these cells that originated in the bone marrow had somehow crept into the brain and taken on the role of microglia in the immune system.
“This suggests that cells are migrating from the blood to the brain,” say Jaiswa. “It’s a remarkable finding.”
“One hypothesis is that the mutations that promote a growth advantage in blood stem cells also promote microglial expansion and activity, boosting the ability of microglia to fight the conditions that lead to brain disease,” Jaiswa continues.
Dysfunction of the brain’s immune system plays a role probable role in Alzheimer’s disease. So if bone marrow impostors do indeed enter the brain in CHIP carriers, they could out-compete the defective brain-derived microglia in Alzheimer’s patients and assume the role that the microglia now neglect.
Oddly enough, the team found no consistent epigenetic changes that would explain these effects when they tried to look. This may be due to the small sample size or whether some other factor is required to trigger them, that has been seen in other disease states, they explain.
So they can’t pin the protection directly to the rogue microglia just yet.
While much remains to be sorted out, the multiple lines of evidence presented by Bouzid and colleagues suggest that bone marrow-derived cells with the CHIP mutations offer some protection against Alzheimer’s disease.
This research was published in Naturopathy.