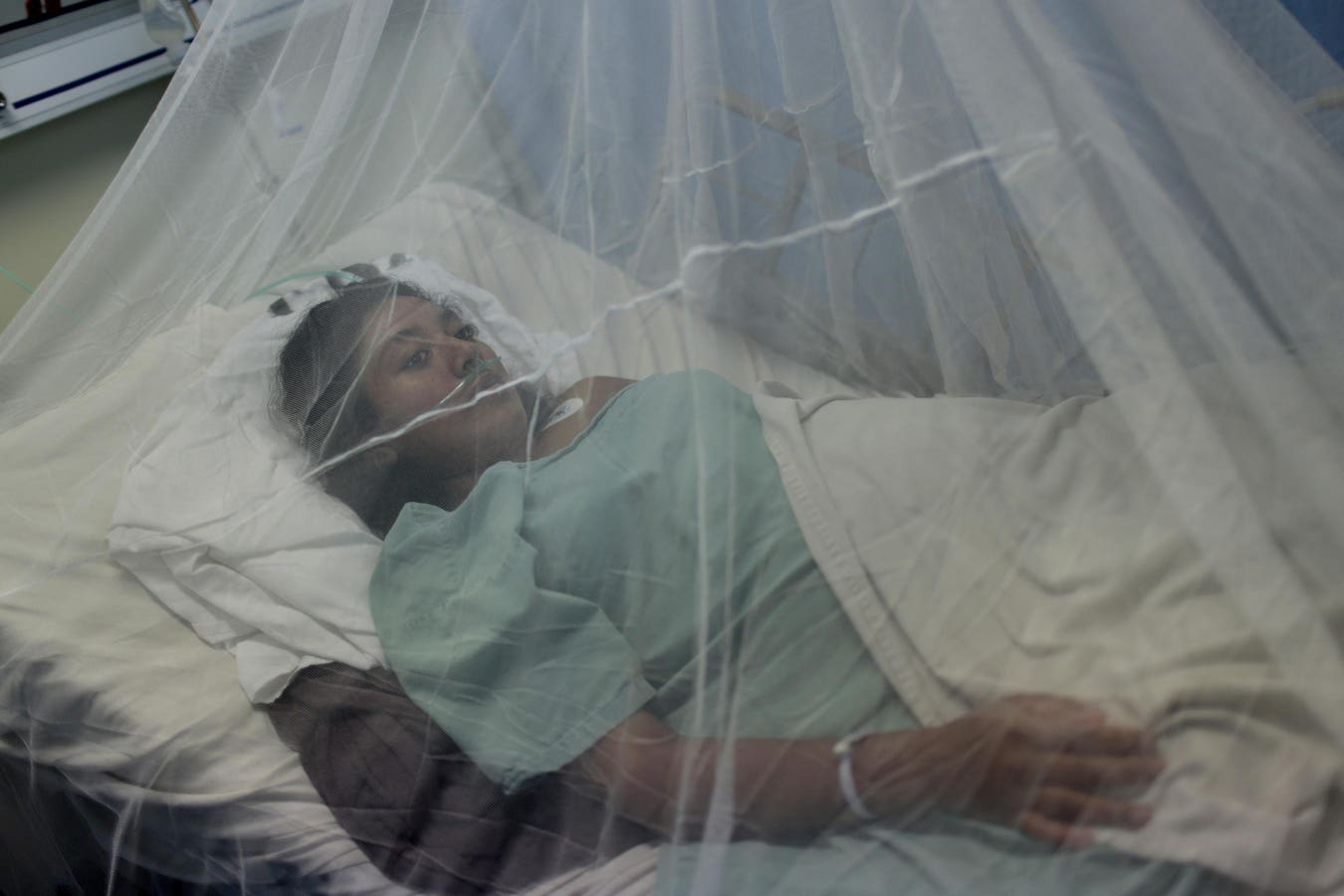
A patient infected with Chikungunya remains in a hospital of Acapulco, Guerrero State, Mexico on … [+]
The Food and Drug Administration recently approved a vaccine against chikungunya (pronounced chi-kuhn-goo-nyuh), a virus spread by mosquitoes in tropical areas across the globe. Most infections are mild and patients recover, but there are reasons having a vaccine makes sense: chikungunya spreads like wildfire, there is no treatment and it can cause devastating long-term disability. Prevention is our best defense.
The Disease
Chikungunya virus causes a disease similar to dengue fever, with high fever, headache, pain behind the eyes, sore throat, fatigue, body aches, joint pains and a red, spotty rash. Symptoms resolve for most people after a week to 10 days, but debilitating joint pain can persist for months or longer in others. The name chikungunya, from the Maconde language of eastern Africa, means “that which bends up,” which is appropriate for a disease that causes people to double over from pain.
The Vaccine
The single-dose vaccine, named Ixchiq, is the first approved vaccine in the U.S. against chikungunya. Adults 18 years of age or older who are at risk of disease are eligible to receive it. The vaccine contains live-attenuated virus, meaning the virus in the vaccine does not reproduce as efficiently as the natural chikungunya virus, but it can cause mild symptoms similar to actual infection. Common vaccine side effects included “headache, fatigue, muscle pain, joint pain, fever, nausea and tenderness at the injection site.”
How Does It Spread?
Chikungunya causes explosive outbreaks spread by Aedes mosquitoes. These mosquitoes are found worldwide, bite during the day and also spread zika and dengue viruses. They are different than Anopheles mosquitoes that spread malaria and generally bite from dusk until dawn. Aedes mosquitoes reproduce in discarded tires and other vessels containing water around the home. The historically efficient vector was Aedes aegypti; however, an interesting phenomenon occurred in 2005. There was a slight alteration of the virus genome, which allowed it to spread more efficiently with a more common mosquito, Aedes albopictus. That facilitated a massive pandemic in 2005 on La Réunion island and neighboring areas around the Indian Ocean. In 2013, chikungunya arrived in the Americas for the first time and it subsequently tore through the Caribbean islands.
Is The United States At Risk?
Yes. Before 2006, chikungunya rarely occurred in U.S. travelers. Then between 2006-2013, we had about 28 cases per year, but those cases were infected outside the U.S. The situation changed after the Caribbean outbreak and chikungunya arrived at our shores in 2014, with affected areas in Florida, the U.S. Virgin Islands and more severely in Puerto Rico (over 30,000 suspected cases).
The continental U.S. dodged a bullet, though, with fewer cases than feared. It probably helps that we have widespread air conditioning and window screens in our southern states, which reduces contact with mosquitoes. We remain vulnerable, though, since we still have the mosquito vectors, primarily in the central and southeast parts of the United States.
How Can I Reduce My Risk?
Minimizing risk focuses on avoiding mosquito bites when living in or visiting an area with active spread of chikungunya, including staying indoors in screened areas during the daytime, using bed nets, using insect repellant and wearing long, loose-fitting clothing. By avoiding Aedes mosquitoes, you reduce your risk of infection from chikungunya as well as dengue and zika viruses.
Do I Need The Vaccine?
If you live in an area with possible exposure to Aedes mosquitoes with active chikungunya spread or are traveling to an at-risk location in Africa, Southeast Asia, or parts of the Americas with ongoing spread, talk to your healthcare provider about possibly getting the vaccine.